Patient positioning sounds like the dullest chapter of a nursing textbook—until you realize the wrong angle can turn a three-day ICU stay into a three-week saga. Enter the thirty-degree lateral inclined position: the Goldilocks tilt that’s not quite flat-on-your-back, not quite side-snoozing, but just right for keeping lungs clear, pressure ulcers at bay, and stomach contents where they belong. Think of it as the ergonomic office chair of hospital beds—simple, cheap, and weirdly powerful. In the next ten minutes you’ll learn why critical-care teams from Baltimore to Berlin are obsessed with this half-roll, how to pull it off without wrestling your patient like a IKEA mattress, and whether you can steal the trick for your own Netflix-marathon setup (spoiler: you can).
Understanding the 30-Degree Lateral Inclined Position
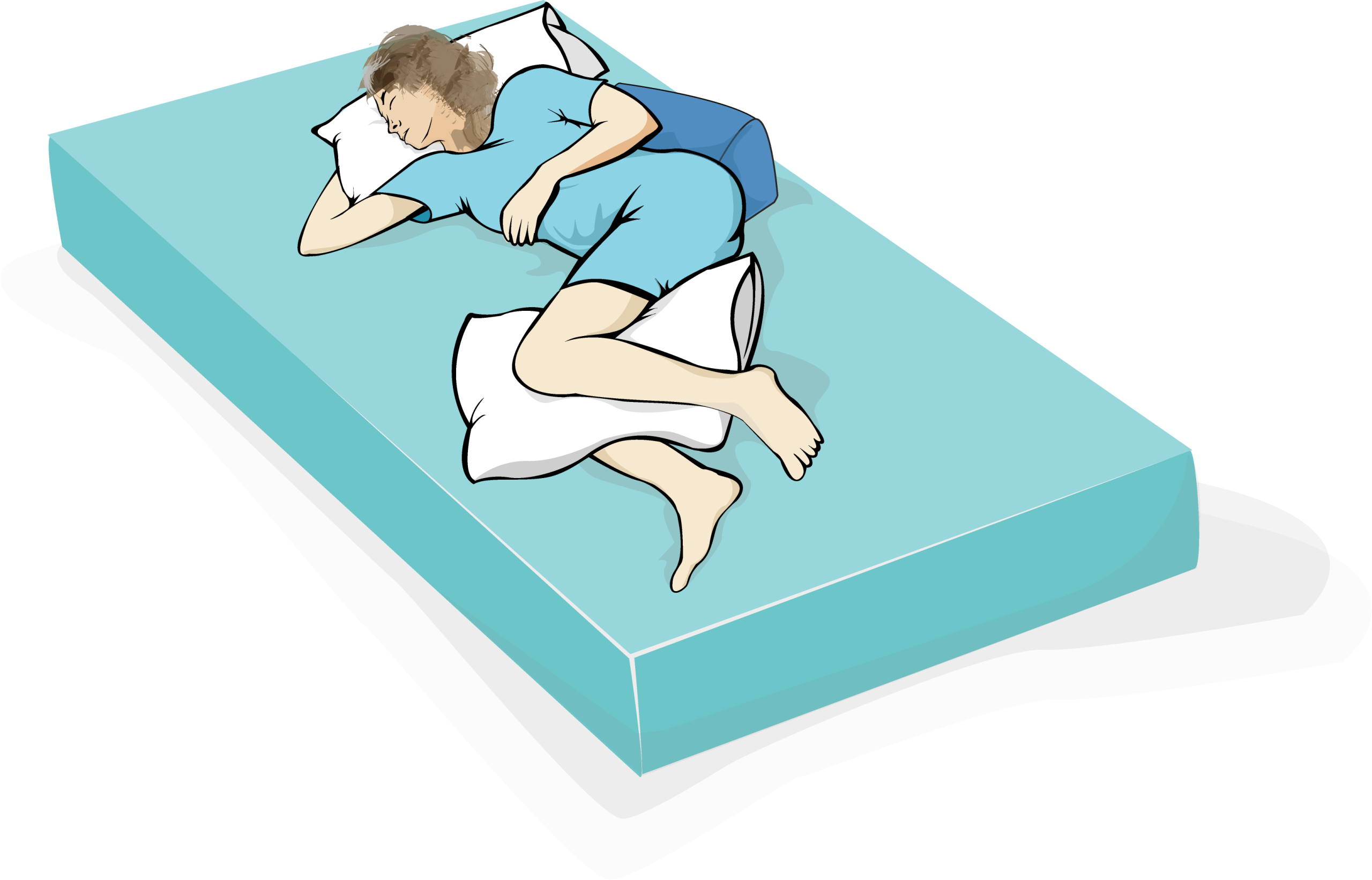
Picture a patient lying on their side—say, the left—but only halfway. The trunk is rotated exactly 30° from the horizontal, the lower shoulder is tucked forward, the upper hip is supported by a firm wedge, and both knees are slightly bent with a pillow between them so bony knees don’t become best friends. The head follows the spine in neutral alignment, like a curious meerkat, not a droopy tulip. In geometry terms, draw an imaginary line from the sternum to the bed surface; that angle should read thirty degrees, not twenty-nine, not thirty-one. ICU nurses sometimes call it the “30-degree shuffle,” because anything steeper turns into full lateral, and anything flatter is basically supine with commitment issues.
Contrast this with the classic positions: supine (flat like a pizza box), full lateral (90°—the fetal sleepers’ delight), prone (face-down “swimmer”), Fowler’s (sitting up 45-60° like Grandpa’s recliner), and Semi-Fowler’s (30-45°). Each has its moment, but none multitask as elegantly as the thirty-degree lateral incline when the goal is “keep lungs open, skin intact, and gastric juice in the stomach.”
Core Medical Applications and Clinical Uses
Ventilator-associated pneumonia (VAP) prevention: The CDC bundles this tilt right next to hand hygiene and oral care. Why? Secretions pool in the posterior oropharynx when you’re flat; gravity plus 30° lets them slide toward the stomach instead of the lungs. A 2019 meta-analysis in Critical Care Medicine showed VAP rates drop by up to 32% when the 30-degree lateral inclined position is rotated every four hours compared with standard supine care.
Aspiration risk: Post-stroke patients with sluggish swallowing, or anyone getting tube feeds at 2 a.m., benefits because the gastro-esophageal junction sits above the glottis. Think of it as putting the cereal bowl on the top shelf so the sleep-walking toddler can’t reach.
Post-op jackpot: After abdominal surgery the tilt unloads the incision from the weight of the viscera; after thoracotomy it lets the “good” lung hang uppermost for better expansion; after craniotomy it can keep intracranial pressure from party-crashing without flattening the cerebral blood flow.
Respiratory management: The upper lung ventilates better, secretions ride the gravitational elevator outward, and oxygenation perks up—handy when your patient’s SATs are flirting with 88%.
Pressure-injury dodge: The sacrum and heels, VIPs (Very Important Pressure points), get a break every time you roll. Rotate side-to-side every two to four hours and you’ve essentially scheduled micro-vacations for the skin.
Neuro tweaks: In traumatic brain injury, a 30° tilt (often combined with head-of-bed elevation) can lower ICP by 3–5 mmHg—about the same relief you feel when you loosen your belt after Thanksgiving, but for the skull.
GI perks: Gastric emptying speeds up because the pylorus faces downhill; reflux episodes fall by roughly 25% according to a Johns Hopkins GI physiology lab study.
Key Benefits and Clinical Advantages
Evidence in plain English: Multiple RCTs show fewer pneumonias, fewer aspiration events, and shorter ICU stays. One study equated the savings to “one less week on a ventilator for every eight patients treated.” That’s the ICU version of a buy-one-get-one deal.
Physiology win: Lung compliance improves, diaphragmatic excursion increases, and the V/Q (ventilation-perfusion) mismatch corrects itself—translation: easier breathing, less wheezy drama.
Comfort upgrade: Patients report less “stuck-in-cement” feeling than supine and less shoulder crunch than full lateral. It’s the difference between economy and premium economy—same cabin, happier hips.
Safety flex: Compared with prone positioning (which needs four people and a choreography rehearsal), the 30-degree tilt can be done single-handedly, reducing staff injury and face-plant accidents.
Practicality: Wedges cost less than a large pizza; no fancy electronics, no app updates, no subscription fees.
Implementation: A Step-by-Step Practical Guide
1. Prep: Explain to the patient—unless they’re sedated, in which case explain to their eyebrows. Gather two firm positioning wedges, one pillow for under the head, one between knees, and possibly a silky draw-sheet to reduce friction.
2. Roll: With a colleague, perform a “log-roll” toward you until the patient’s back is 30° off the bed. Slide the wedge behind the back, tucking it from scapula to hip so the angle holds.
3. Align: Lower shoulder pulled slightly forward to avoid brachial-plexus yoga. Head on pillow in neutral. Upper leg forward, knee bent, resting on pillow; lower leg straight-ish.
4. Secure: Check that hips and shoulders stack like Jenga blocks, not twisted like a pretzel. Use a small second wedge under the abdomen if the patient is bariatric to prevent sag.
5. Monitor: Skin every two hours, SpO₂ trends, endotracheal-tube depth, and patient grimace scale (a.k.a. “ouch face”). Document angle, time, and any “red-flag” numbness or tingling.
6. Rotate: Alternate sides every two to four hours, or follow unit protocol. If spinal precautions exist, skip the twist and use a specialty bed that achieves the angle instead.
Contraindications: Unstable spinal injuries without clearance, open pelvic trauma with external fixation, certain limb fractures that rotate=agony, and the rare patient whose intracranial pressure paradoxically rises with elevation (yes, they exist—physiology loves curveballs).
Supporting Evidence, Research, and Guidelines
The CDC’s VAP prevention guidelines list semi-recumbent plus lateral rotation as a core bundle element. The WHO’s 2020 SAVE LIVES: Clean Care campaign echoes the 30–45° head-of-bed angle, and many ICUs layer the lateral tilt on top. A landmark 2018 Intensive Care Medicine RCT of 1,200 ventilated patients found the lateral-rotation group had 7.2 ventilator-days versus 9.4 in the supine group. Even Mayo Clinic’s pressure-ulcer primer recommends scheduled lateral turns as a Grade 1A intervention—fancy code for “just do it.”
Special Considerations and Protocol Variations
Pediatrics: Use smaller, pediatric-specific wedges; angle can be eyeballed with a phone-level app—because Gen-Z nurses measure everything with smartphones anyway.
Neonates: Consider “nest” boundaries so the 30° roll doesn’t turn into 60° break-dance.
Bariatrics: Add an extra wedge under the panniculus to prevent the torso from sliding downhill like a glacier.
Elderly with osteoporosis: Pad the upper shoulder generously; their scapulae can be sharper than your ex’s tongue.
Bundle buddies: Combine with chlorhexidine oral care, sub-glottic suctioning, and early mobility. Think of it as the Avengers lineup—each hero okay alone, unstoppable together.
Angle flexibility: 25–35° is acceptable in real life; aim for 30° like you aim for 10,000 steps—close enough counts.
Frequently Asked Questions (FAQ)
Is 30 degrees measured exactly, or is a range acceptable? ICU police won’t write you a ticket for 28°, but keep it between 25–35°. Pro-tip: most phone inclinometers are accurate to ±2°—just disinfect the case afterward.
How does this position help prevent pneumonia exactly? Gravity drains oral and gastric secretions toward the gut, away from the trachea, while the upper lung ventilates better. Fewer germs in the airway equals fewer infections—like keeping rainwater out of your basement.
Can this position be used for all patients on bed rest? Almost all. Exceptions: unstable spine, certain pelvic or limb fractures, and some ICP quirks. When in doubt, ask the attending or the trauma gods.
How often should a patient in this position be repositioned? Every 2–4 hours side-to-side, or per unit policy. Skin checks happen each time—think of it as scheduled snack breaks for tissue viability.
What is the main difference between this and just elevating the head of the bed? Head-of-bed elevation is “sit-up”; lateral incline is “half-roll.” Combine them and you get the best of both: secretions drain down, sacrum unloads, and nurses smile more.
Are there any risks if the position is done incorrectly? Sure—brachial-plexus stretch, hip rotation contractures, or the wedge slipping and turning 30° into 0° real quick. Proper support and monitoring are cheaper than lawsuit settlements.
Conclusion
The thirty-degree lateral inclined position is the unsung hero of patient care: no batteries, no billion-dollar patent, just a humble wedge and a bit of geometry saving lungs, skin, and stomachs every shift. It’s the clinical equivalent of flossing—quick, inexpensive, and annoyingly effective. Whether you’re a bedside nurse, a respiratory therapist, or a savvy at-home caregiver, mastering this tilt means you’re wielding evidence-based medicine in its simplest form. So grab a wedge, level up that smartphone app, and roll your patients (or yourself) into the sweet spot where physiology sighs in relief and complications think twice about crashing the party.
References and Further Reading
CDC Ventilator-Associated Pneumonia Prevention Guidelines
WHO Guidelines on Core Components Infection Prevention
Mayo Clinic: Pressure Ulcers Overview
Healthline: VAP Causes and Prevention
Compendium of Physical Activities and Critical Care Nursing Textbooks (used by clinicians for energy-expenditure and positioning data).