Picture this: you’re in the bathroom for the third time in an hour, wincing like you just bit into a lemon. Is it a pesky urinary-tract infection (UTI) or something more sinister—say, a sexually transmitted infection (STI) masquerading as one? Before you spiral into WebMD-induced panic, breathe. This article is your no-judgment guide to spotting the difference, taking a quick self-check quiz, and figuring out what to do next—without the awkward small talk with Dr. Google.
Quick disclaimer before we dive in: nothing here replaces a real-live clinician. The quiz is a sorting hat, not a lab coat. If it burns, bleeds, or blisters, get thee to a licensed provider.
1. UTI vs. STD: Understanding the Core Differences
1.1 What is a UTI? Common Causes and Symptoms
A UTI is basically a bacterial block party in your urinary tract—usually E. coli plus friends. Think of it as the frat house of infections: loud, messy, and impossible to ignore.
- Burning or stinging when you pee (the classic “peeing razor blades” line).
- Constant urge to go, even when your bladder feels emptier than your Netflix queue.
- Cloudy, funky-smelling urine—like someone poured a craft beer in the toilet.
- Low pelvic ache that makes you want to curl up with a heating pad and a pint of ice cream.
1.2 What is an STD? Overview and Key Types
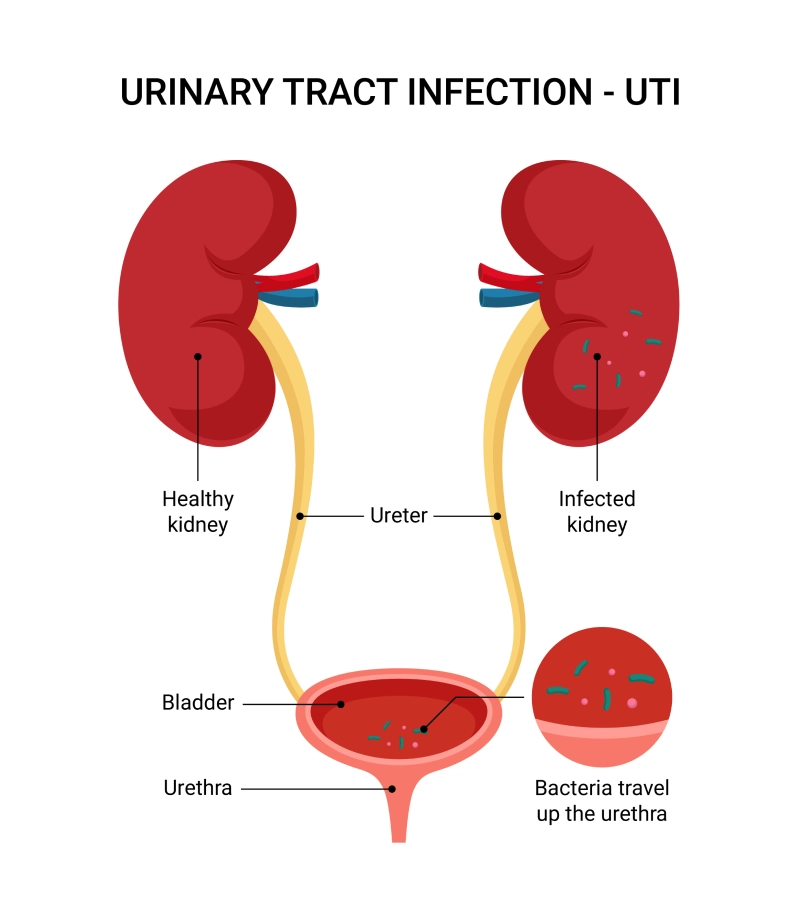
STDs (or STIs, if you prefer the newer, trendier acronym) are infections you pick up through sexual contact—vaginal, anal, oral, or shared toys. Some, like chlamydia and gonorrhea, mimic UTI symptoms so well they deserve an Oscar. Others—herpes, HPV, syphilis, HIV—bring their own unique drama (sores, warts, rashes, flu-like misery).
1.3 Side-by-Side Symptom Comparison Chart
| Symptom | UTI | Chlamydia/Gonorrhea | Herpes |
|---|---|---|---|
| Burning on urination | Yes, front-and-center | Yes, can be identical | Sometimes, especially if sores near urethra |
| Frequent/urgent need to pee | Yes | Often | Less common |
| Abnormal genital discharge | Rare | Yes—yellow, green, or white | Clear or pus-like from sores |
| Pelvic/bladder pain | Low abdomen/bladder | Lower abdomen, can radiate | Pubic area, buttocks, thighs |
| Visible sores or blisters | No | No | Yes—clustered blisters |
| Partner with symptoms | Not relevant | Often yes | Possibly |
2. The Self-Assessment Quiz: Key Questions Explained
2.1 How the Quiz Works
Answer honestly—no one’s peeking over your shoulder. Each question funnels you toward one of three buckets: “Likely UTI,” “Possible STD,” or “Call the doctor now.” Keep a mental tally or scribble on your phone.
2.2 Core Quiz Question Categories
Symptom Profile
- How long have you felt the burn? (<24 h, 1–3 days, >3 days)
- Rate the pain: 1 = “meh,” 5 = “I’m pricing candles for my urethra’s memorial service.”
- Any blood in urine, sores, or weird discharge?
Sexual History & Protection
- New partner(s) in the past 60 days?
- Condom use: always, sometimes, never, or “what’s a condom?”
- Partner(s) mention any symptoms or positive tests?
Personal Medical History
- Previous UTIs or STIs—how many and when?
- Currently pregnant, immunocompromised, or diabetic?
- Recent antibiotic use (can mask infections)?
3. Interpreting Your Quiz Results and Understanding Limitations
3.1 Possible Result Categories
- Likely UTI: classic urinary symptoms, minimal risk factors for STDs.
- STD Risk Possible: any sexual risk factor plus urinary symptoms, or unexplained discharge/sores.
- Seek Immediate Care: fever >101 °F, back/flank pain, pregnancy, or severe pain with visible sores.
3.2 What Your Results Really Mean
Think of your result as the “check engine” light, not the mechanic’s invoice. A “Likely UTI” still needs a urine culture; chlamydia can lurk quietly for months. A “Possible STD” means it’s time to pause the bedroom Olympics and get screened.
3.3 The Crucial Limits of an Online Quiz
Up to 70 % of chlamydia cases in women are asymptomatic. Meanwhile, over-the-counter UTI test strips miss up to 25 % of real infections. Translation: negative quiz ≠ hall pass. Only a lab can say “yea” or “nay.”
4. Your Action Plan: Next Steps Based on Your Assessment
4.1 If Your Results Suggest a UTI
Home TLC:
- Chug water like you’re in a desert TikTok challenge—2–3 L daily.
- Try phenazopyridine (AZO) for temporary pain relief; warning: it turns urine traffic-cone orange.
- Cranberry capsules (not sugary juice) may block bacterial Velcro, per a Mayo Clinic review.
When to escalate: symptoms >48 h, fever, back pain, or pregnancy. Expect a urinalysis, maybe a culture, and first-line antibiotics like nitrofurantoin.
4.2 If Your Results Suggest a Possible STD
- Hit pause on sex. Yes, even “just oral.” Even if you “totally trust them.”
- Notify partners. Apps like SuggestATell or anonymous text services can do the dirty work for you.
- Get tested. Most clinics offer combo panels: urine for chlamydia/gonorrhea, blood for HIV/syphilis, swab for herpes if sores present. The CDC’s GetTested locator shows free or low-cost sites near you.
4.3 Red Flags: When to Seek Immediate Medical Care
- Fever >101 °F with flank pain—possible kidney infection or pelvic inflammatory disease.
- Nausea/vomiting preventing you from keeping down fluids or meds.
- Pregnancy plus any urinary symptoms—UTIs can trigger preterm labor.
- Testicular or scrotal pain in penis-owners—rule out epididymitis.
5. Prevention and Long-Term Sexual & Urinary Health
5.1 Preventing UTIs
- Pee after sex—think of it as the post-coital rinse cycle.
- Wipe front-to-back; your mom was right.
- Stay hydrated enough that your pee looks like “pale straw,” not IPA beer.
- If you get >3 UTIs a year, ask about low-dose prophylactic antibiotics or methenamine hippurate.
5.2 Preventing STDs
- Condoms, used correctly, slash chlamydia/gonorrhea risk by >90 %. Keep a variety pack handy—no one likes a late-night pharmacy run.
- Talk before you rock: swap last test dates like Spotify playlists.
- Vaccines: HPV (Gardasil 9) up to age 45, plus Hepatitis B series if you missed it in school.
5.3 The Importance of Regular Screenings
The CDC recommends annual chlamydia/gonorrhea screens for all sexually active women <25 and older women with risk factors. Men who have sex with men should test every 3–6 months if HIV-negative and having new or multiple partners. Schedule it like a dental cleaning—only with less floss.
6. Frequently Asked Questions (FAQ)
Can a UTI be mistaken for an STD (and vice versa) by a doctor?
Absolutely. A 2020 Journal of Emergency Medicine study found 18 % of women diagnosed with “UTI” actually had chlamydia. Labs don’t lie.
Can sexual activity cause a UTI?
Yup. “Honeymoon cystitis” is real—friction can scoot bacteria toward the urethra. Pee, rinse, repeat.
I have no symptoms. Could I still have an STD?
See: chlamydia, HPV, HIV early days, syphilis—silent but deadly (or at least annoying). Screen anyway.
How soon after exposure can STD symptoms appear?
Chlamydia: 1–3 weeks. Gonorrhea: 2 days–2 weeks. Herpes: 2–12 days. HIV: 2–4 weeks (flu-like). Syphilis: 10–90 days.
Are online or at-home test kits reliable?
FDA-approved kits (Everlywell, LetsGetChecked) hover around 95 % accuracy—if you collect the sample correctly. Follow the swab like it’s a sour-dough recipe.
What happens if I leave a UTI or STD untreated?
UTI can march to your kidneys; STDs can scar your tubes, tank your fertility, or inflame your joints. Treatment beats regret.
7. Resources and Further Reading
- CDC – Sexually Transmitted Diseases
- Planned Parenthood – STD Info
- American Sexual Health Association
- National STD Hotline: 1-800-232-4636 (free, confidential)
Conclusion
So, do you have a UTI or an STD? The quiz can steer you toward the most likely suspect, but the final verdict comes from a lab, not a laptop. Whether it’s a quick round of antibiotics or a round of partner notifications, both conditions are routine, treatable, and nothing to be ashamed of. Book the appointment, pee in the cup, swab the sore, and then get back to living your life—preferly hydrated, protected, and a little bit wiser.